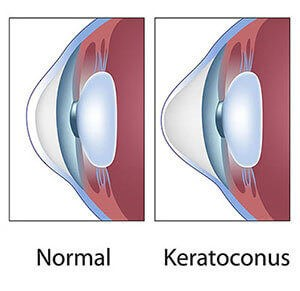
Keratoconus Treatment and Management
Corneal Cross-Linking (CXL)
Corneal cross-linking is a minimally invasive outpatient procedure designed to treat progressive keratoconus (and, sometimes, other conditions that cause a similar weakening of the cornea).
The corneal cross-linking procedure strengthens and stabilise the cornea by creating new links between collagen fibers within the cornea. The two-step procedure applies specialty formulated riboflavin (vitamin B) eye drops to the surface of the eye immediately followed by a controlled exposure of the eye to ultraviolet light.
Corneal cross-linking can be combined with other procedures for keratoconus treatment. For example, it can be performed along with implantation of tiny arc-shaped corneal inserts called INTACS to reshape and stabilise the cornea in more advanced cases of keratoconus.
Intracorneal Rings (INTACS)
INTACS corneal inserts or implants are a minimally invasive surgical option used primarily for the treatment of keratoconus. INTACS are two tiny, clear crescent-shaped pieces of a plastic polymer that are inserted into the cornea to reshape the front surface of the eye.
Full Thickness Corneal Transplant
Your entire cornea may need to be replaced if both the front and inner corneal layers are damaged. This is called penetrating keratoplasty (PK), or full thickness corneal transplant. Your diseased or damaged cornea is removed. Then the clear donor cornea is sewn into place.
PK has a longer recovery period than other types of corneal transplants. Getting complete vision back after PK may take up to one year or longer.
With a PK, there is a slightly higher risk than with other types of corneal transplants that the cornea will be rejected. This is when the body’s immune system attacks the new cornea tissue.
Partial Thickness Corneal Transplant
Sometimes the front and middle layers of the cornea are damaged. In this case, only those layers are removed. The endothelial layer, or the thin back layer, is kept in place. This transplant is called deep anterior lamellar keratoplasty (DALK) or partial thickness corneal transplant. DALK is commonly used to treat keratoconus or bulging of the cornea.
Healing time after DALK is shorter than after a full corneal transplant. There is also less risk of having the new cornea rejected.
Endothelial Keratoplasty
In some eye conditions, the innermost layer of the cornea called the “endothelium” is damaged. This causes the cornea to swell, affecting your vision. Endothelial keratoplasty is a surgery to replace this layer of the cornea with healthy donor tissue. It is known as a partial transplant since only this inner layer of tissue is replaced.
There are a few types of endothelial keratoplasty. They are known as:
-
DSEK (or DSAEK) — Descemet's Stripping (Automated) Endothelial Keratoplasty
-
DMEK — Descemet's Membrane Endothelial Keratoplasty
Each type removes damaged cells from an inner layer of the cornea called Descemet’s membrane. The damaged corneal layer is removed through a small incision. Then the new tissue is put in place. Just a few stitches are needed to close the incision. Much of the cornea is left untouched. This lowers the risk of having the new cornea cells being rejected after surgery.
Meet our Specialist
Dr Ainur Rahman Dato Setia Dr Anuar Masduki
Designation
Consultant Ophthalmologist and Corneal Surgeon






